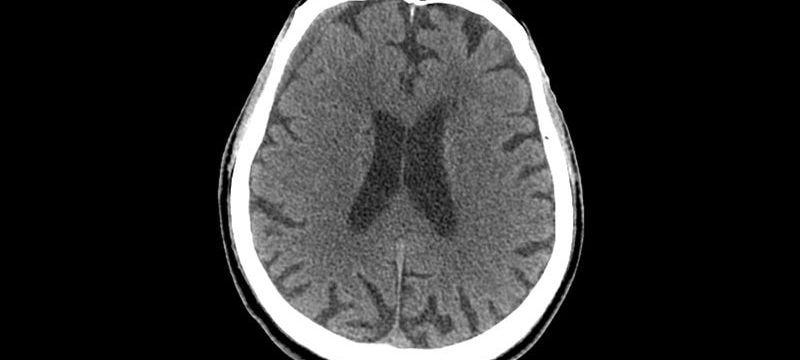
LOS ANGELES — Patients with supratentorial intracerebral hemorrhage (ICH) had better outcomes when they were treated with a form of minimally invasive surgery to remove clots instead of with standard care, a new study finds.
Results of a randomized trial show that patients who underwent minimally invasive trans-sulcal, parafascicular surgery (MIPS) after supratentorial ICH had a slightly lower mortality rate at 6 months (20.0%) than the standard care group (23.3%).
The surgery group also scored better on the utility-weighted modified Rankin score, the primary endpoint (0.458 vs 0.374; difference = 0.084.)
The clot evacuation procedure “gets in, gets the job done, and prevents the nasty consequences of having a blood clot. And it doesn’t cause damage to the patient,” said study lead author Gustavo Pradilla, MD, a neurosurgeon at Emory University School of Medicine, Atlanta, Georgia, in an interview.
The results of the Early Minimally Invasive Removal of Intracerebral Hemorrhage (ENRICH) trial were presented at the American Association of Neurological Surgeons (AANS) 2023 Annual Meeting.
Supratentorial intracerebral hemorrhage makes up 10% to 15% of all strokes, the authors note. These strokes occur when hemorrhage begins in the main tissue of the brain. One major risk is that the bleeding can damage the brain by causing pressure to build up within the skull.
Neurosurgeons often avoid giving thrombolytics to patients with hemorrhagic strokes because they can cause even more bleeding. But, as Pradilla explained, clots can still be dangerous in these patients because the body can respond to them by boosting inflammation. As a result, “the brain goes into uncontrollable swelling” and many patients deteriorate in intensive care.
The new randomized, multicenter, adaptive trial examined MIPS using devices manufactured by the NICO Corporation, which funded the trial. BrainPath is a device to provide trans-sulcal access to the brain and the Myriad device then evacuates the hemorrhage. “As a result, the brain will no longer be dealing with that large amount of clot,” he said.
Researchers recruited patients between 2016 and 2022 at 37 centers. All had strokes in basal ganglia or lobar locations and were eligible if surgery was performed within 24 hours of their last-known normal. Centers in the trial were encouraged to perform the procedure within 8 hours, Pradilla said.
The utility-weighted modified Rankin score analysis included 139 patients treated with standard care (mean age, 61.5 years; 52% female; 69% white) and 147 in the MIPS group (mean age, 62.6 years; 48% female; 71% white).
While the surgical patients had better outcomes overall, the difference was only positive in the lobar group (+0.1418). The basal ganglia group fared worse (-0.0406).
Regarding adverse effects, “we didn’t have any safety concerns” in previous pivotal research, he said. And, he noted, the devices are already approved by the US Food and Drug Administration.
As for cost, Pradilla said researchers are examining the expense of the procedure, given the prospect that patients will need less intensive care because of improved outcomes. “One of the things we’re trying to prove is that there is an economic benefit,” he said.
In an interview, neurosurgeon Wendy Ziai, MD, MPH, Johns Hopkins Medicine, Baltimore, Maryland, said the study results are “very encouraging” and confirm the findings of previous trials.
Still, she said, there’s a “need for a large, definitive trial.” She cautioned that improvements as measured by the Rankin score analysis are “relatively minor,” and “one should ask whether this degree of change is likely to be beneficial to patients.”
The importance of the difference in mortality, she added, is uncertain.
Going forward, she said, “we need better descriptions of who benefits from minimally invasive surgery and how much the benefit is from the survivor perspective. Also, what is the time window for surgery? Does the surgical technique matter, or is the benefit independent of technique but reliant on the removal of clot?”
Still, she said, “this trial seems to be evidence that removal of clot is a truly important goal.”
American Association of Neurological Surgeons (AANS) 2023 Annual Meeting. Presented April 22, 2022.
NICO Corporation funded the trial. Disclosures for study authors were not provided. Ziai has received grants from the National Institutes of Health to study intracerebral hemorrhagic strokes. Pradilla discloses research funding from the Acoustic Neuroma Association, the Emory Medical Care Foundation, and NICO Corporation, and consulting work for Stryker and Aesculap.
For more Medscape Neurology news, join us on Facebook and Twitter.
Source: Read Full Article