Spinal cord stimulation (SCS) for chronic pain involves delivering low levels of electricity directly into the spinal cord using an implanted device, which modifies or blocks nerve activity to minimize the sensation of pain reaching the brain. The approach is most often used after nonsurgical pain treatment options have failed to provide sufficient relief.
The underlying mechanisms of how SCS works are not fully understood, but in a new paper published in the April 28, 2022 online issue of the journal Bioelectronic Medicine, a research team led by scientists at University of California San Diego School of Medicine report high-frequency SCS proved more effective at improving perceived pain reduction (PPR) than low-frequency SCS in patients studied, and that there was some variation in PPR between male and female patients.
Low-frequency SCS (50 Hz) was originally approved by the U.S. Food and Drug Administration (FDA) as a treatment for intractable back and leg pain in 1989. In 2015, the FDA approved high-frequency SCS (10,000 Hz), which delivers electrical stimulation pulses that are shorter in duration, lower in amplitude and do not induce paresthesia, the abnormal sensation of tingling or prickling.
The newly published retrospective study examined 237 patients who had received SCS treatment between 2004 and 2020: 94 patients (40 females, 54 males) who received HF-SCS and 143 patients (70 females and 73 males) who received LF-SCS. At three and six months post-implantation, the researchers found that PPR across all patients improved compared to baseline, but HF-SCS produced greater PPR than LF-SCS. HF-SCS was also associated with less subsequent use of opioids to mitigate pain.
However, there were differences in the findings between sexes:
- Male PPR, for example, was significantly better for HF-SCS at three and six months when compared to LF-SCS, while this was only true for females at the six-month time point.
- LF-SCS males used more opioids post-implantation and at six months while females used more opioids post-implantation, at three, six and tended to use more opiates at the 12-month time-point.
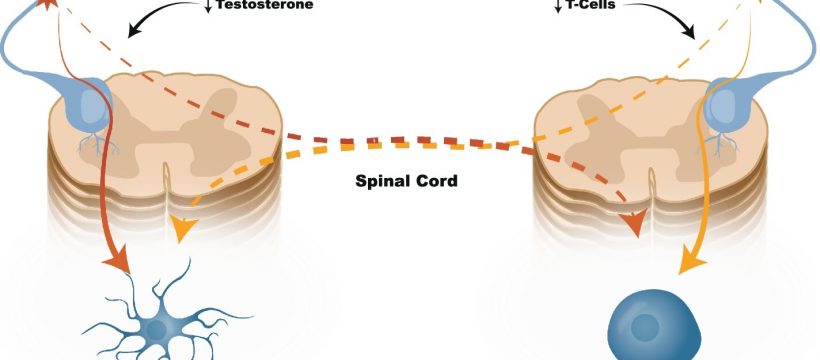
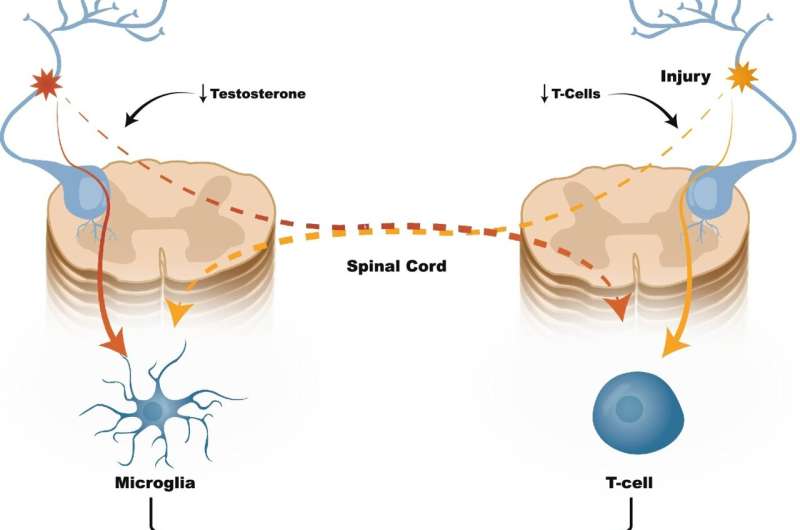
“Our work was sparked by a growing literature that demonstrate sex specific immune pathways differentially contribute to chronic pain processes,” said senior author Imanuel Lerman, MD, an associate professor of anesthesiology, pain management specialist at UC San Diego Health, and an affiliate of the Qualcomm Institute. “The observed parameter-specific (high versus low frequency) sex-based differences in spinal cord stimulation efficacy and opiate use are definitely intriguing.
Source: Read Full Article