
In the past 10 years, the percentage of Americans who use medical marijuana has more than doubled as state-level legalization becomes increasingly common. But despite its prevalence as a medication, the full health effects of cannabis remain unknown, especially for specific populations—such as pregnant people—that might be especially at risk of health complications.
Now, in a large study of more than 9,000 pregnant people from across the U.S., researchers at University of Utah Health have found that cannabis exposure during pregnancy is associated with a composite measure of unhealthy pregnancy outcomes, especially low birth weight, and that higher exposure is associated with higher risks.
Compared to most prior studies, this study was larger and measured cannabis exposure more accurately, which allowed researchers to distinguish the effects of cannabis itself from those caused by other correlated health conditions. The research, “Cannabis Exposure and Adverse Pregnancy Outcomes Related to Placental Function,” was published online in JAMA.
“Cannabis use is not safe,” says Robert Silver, M.D., professor of obstetrics and gynecology at U of U Health and last author on the study. “It increases the risk of pregnancy complications. If possible, you shouldn’t use cannabis during pregnancy.”
The researchers were driven to answer this question in part by the contradictory answers that many people encounter when trying to learn about the health impacts of cannabis use.
“There’s so much information out there—discussion and social media channels and on the Internet—about cannabis use and pregnancy,” explains Torri Metz, M.D., vice chair of research of obstetrics and gynecology at U of U Health and lead author on the study. “I think it’s hard for patients to understand what they should be worried about, if anything.”
Uncovering new risks
Indeed, some previous studies on the topic found no association between cannabis use and pregnancy complications. One hurdle facing such research, Metz says, is that there are “so many differences between baseline characteristics of people who use and don’t use cannabis during pregnancy. There’s different rates of anxiety and depression.”
These differences can also impact pregnancy risks, which makes it challenging to figure out the consequences related specifically to cannabis use.
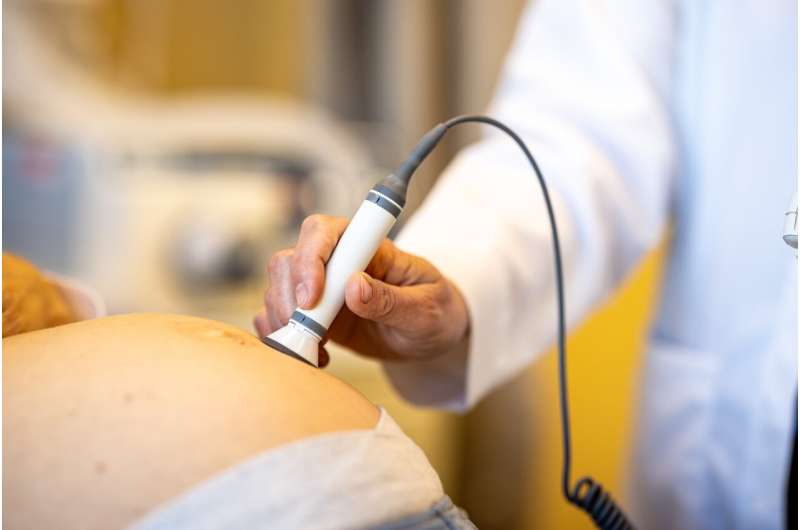
The large study population, including participants from eight medical centers across the U.S., allowed the researchers to address this issue. Being able to compare pregnancy outcomes for so many participants, 610 of which had detectable levels of cannabis exposure, meant that the researchers could statistically untangle the impacts of cannabis use from many other factors, including pre-existing health conditions, nicotine exposure, and socioeconomic status.
The scientists found that cannabis exposure was associated with a 1.5-fold increase in risk: 26% of cannabis-exposed pregnant people experienced an unhealthy pregnancy outcome, versus 17% of non-exposed pregnant people. Higher levels of cannabis exposure over the course of pregnancy were associated with higher risks.
A distinguishing feature of the study was how the researchers measured cannabis exposure. While other studies had asked participants to report their own cannabis use (which has been shown to underestimate the actual rate of use by two or three times), the scientists measured the levels of a metabolic byproduct of cannabis in participants’ urine samples, which gave more accurate measurements of cannabis exposure.
Open questions
To gauge impacts on pregnancy, the researchers looked at an aggregate measure of negative health outcomes, including low birth weight, pregnancy-related high blood pressure, stillbirth, and medically indicated preterm birth. Of these, the association between cannabis use and low birth weight was the strongest. All of these conditions have been linked to reduced function of the placenta, which supplies the growing baby with oxygen and nutrients.
While this type of study can’t determine ‘why’ cannabis is associated with negative pregnancy outcomes, previous studies in non-human primates have found that long-term cannabis exposure can interfere with blood supply to the placenta. The correlation Metz and her colleagues observed suggests that cannabis may disrupt the human placenta in a similar way.
Silver adds that the greater risk seen at higher levels of exposure is especially concerning given the high amount of THC found in newer cannabis products—products that were barely starting to become available from 2010 to 2014, when the study data was collected. The health impacts of these more concentrated products remain largely unknown.
The researchers urge people who are considering using cannabis while pregnant to have an open conversation with their doctor. While pregnant people may turn to cannabis to alleviate nausea or anxiety, other remedies have been proven to be safe. “There are many, many reasons people use cannabis,” Silver says. “But there may be alternative therapies that can help mitigate the symptoms.”
Silver emphasizes that continued research on the health impacts of cannabis is urgently needed so that patients can make informed decisions about their health. “As long as humans are interested in using this product,” he says, “we ought to assess health effects both good and bad, as accurately as we can, and provide that information for folks.”
The research was carried out in collaboration with researchers from ARUP Laboratories, University of California, Irvine, The Ohio State University, Indiana University, Case Western Reserve University, University of Pennsylvania, Columbia University, Eastern Virginia Medical School, and University of Pittsburgh.
More information:
Cannabis Exposure and Adverse Pregnancy Outcomes Related to Placental Function, JAMA (2023). DOI: 10.1001/jama.2023.21146. jamanetwork.com/journals/jama/ … 1001/jama.2023.21146
Journal information:
Journal of the American Medical Association
Source: Read Full Article
